Curriculum
Fellows must be able to provide patient care that is compassionate, appropriate, and effective for the evaluation and treatment of health problems and the promotion of health as it relates to rheumatic diseases; demonstrate knowledge of established and evolving biomedical, clinical, epidemiological and social-behavioral sciences; as well as apply it to patients with rheumatic diseases.
By the end of the fellowship, fellows are expected to:
Learn the practice of health promotion, disease prevention, diagnosis, care and treatment of men and women from adolescence to old age during health and all stages of illness.
Learn the practice of health promotion, disease prevention, diagnosis, care and treatment of men and women from adolescence to old age during health and all stages of illness.
Demonstrate competence in the prevention, evaluation, and management of the following disorders:
- Rheumatoid arthritis
- Systemic lupus erythematosus
- Scleroderma/systemic sclerosis
- Polymyositis
- Pediatric Rheumatic Diseases
- Spondyloarthopathies
- Vasculitis
- Crystal-induced arthritis
- Osteoarthritis
- Regional musculoskeletal pain syndromes and acute and chronic musculoskeletal pain syndromes
- Nonarticular rheumatic diseases, including fibromyalgia
- Nonsurgical, exercise-related (sports) injury
- Systemic diseases with rheumatic manifestation
- Metabolic diseases of bone
- Osteoporosis
- Infection of joints and soft tissues
- Sjögren's syndrome
Demonstrate competence in the prevention, evaluation, and management of the following disorders:
- Rheumatoid arthritis
- Systemic lupus erythematosus
- Scleroderma/systemic sclerosis
- Polymyositis
- Pediatric Rheumatic Diseases
- Spondyloarthopathies
- Vasculitis
- Crystal-induced arthritis
- Osteoarthritis
- Regional musculoskeletal pain syndromes and acute and chronic musculoskeletal pain syndromes
- Nonarticular rheumatic diseases, including fibromyalgia
- Nonsurgical, exercise-related (sports) injury
- Systemic diseases with rheumatic manifestation
- Metabolic diseases of bone
- Osteoporosis
- Infection of joints and soft tissues
- Sjögren's syndrome
Demonstrate competence in performing and/or interpreting basic rheumatologic examination, procedures, injections, and clinical and research studies
Demonstrate competence in performing and/or interpreting basic rheumatologic examination, procedures, injections, and clinical and research studies
Consults and Clinics
First-year fellows will spend five months each year managing the rheumatology consult service on a rotating basis; second-year fellows do one month.
Ambulatory experience through both years of fellowship will consist of two half-day continuity clinics per week.
Research and Conferences
Each fellow is expected to participate in a research project under the supervision of a research mentor, as well as engage in and complete scholarly activity. Fellows are required to attend at least 90 percent of each of the conferences held weekly and monthly.
Private Practice and Ambulatory Experience
The Lexington Clinic provides rheumatology fellows a minimum of one month in private practice rotation in an outpatient setting two to three half-days per week during the second year of fellowship. Fellows will have three to four elective months in each year which provide additional ambulatory experience in a variety of other disciplines including pediatrics, sports medicine, physical medicine and rehabilitation, neurology, pulmonary, nephrology, and bone clinic. Second-year fellows will be allowed to choose elective areas in which they maintain interest or seek further growth.
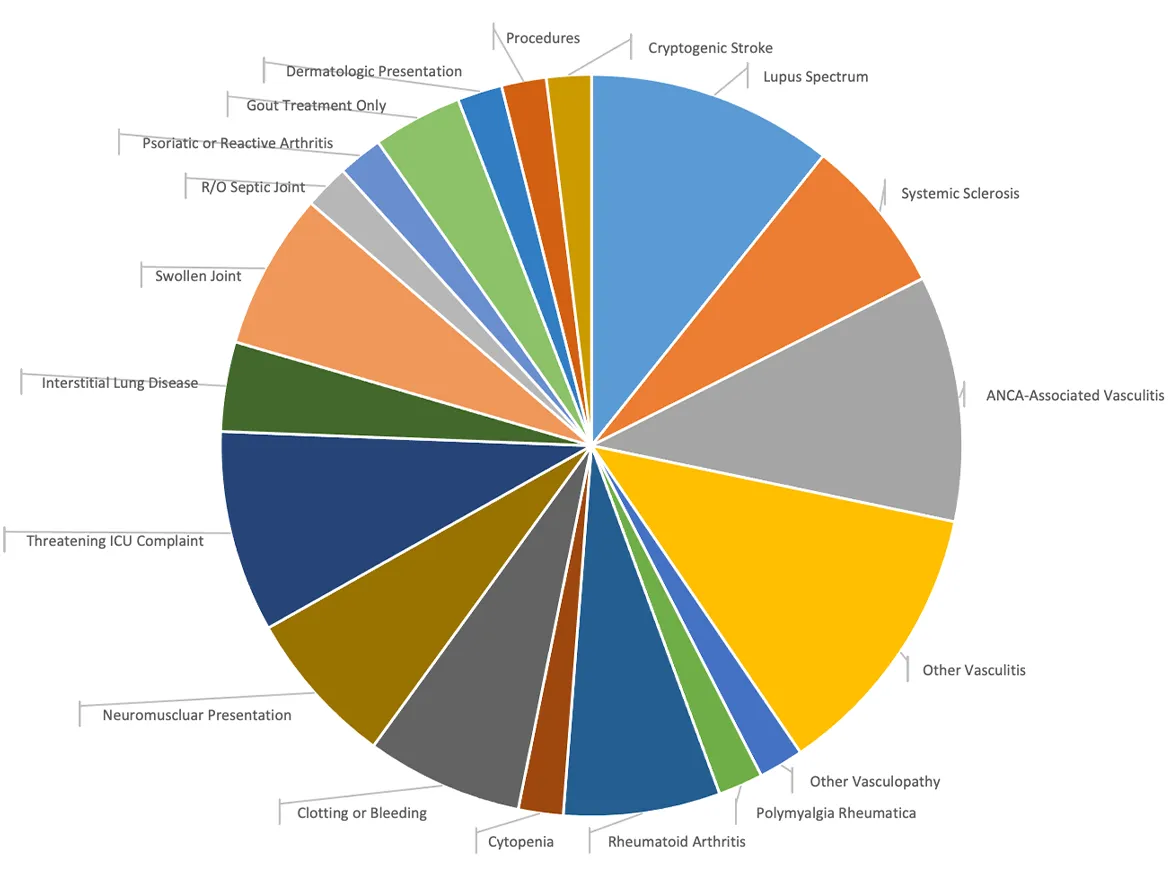
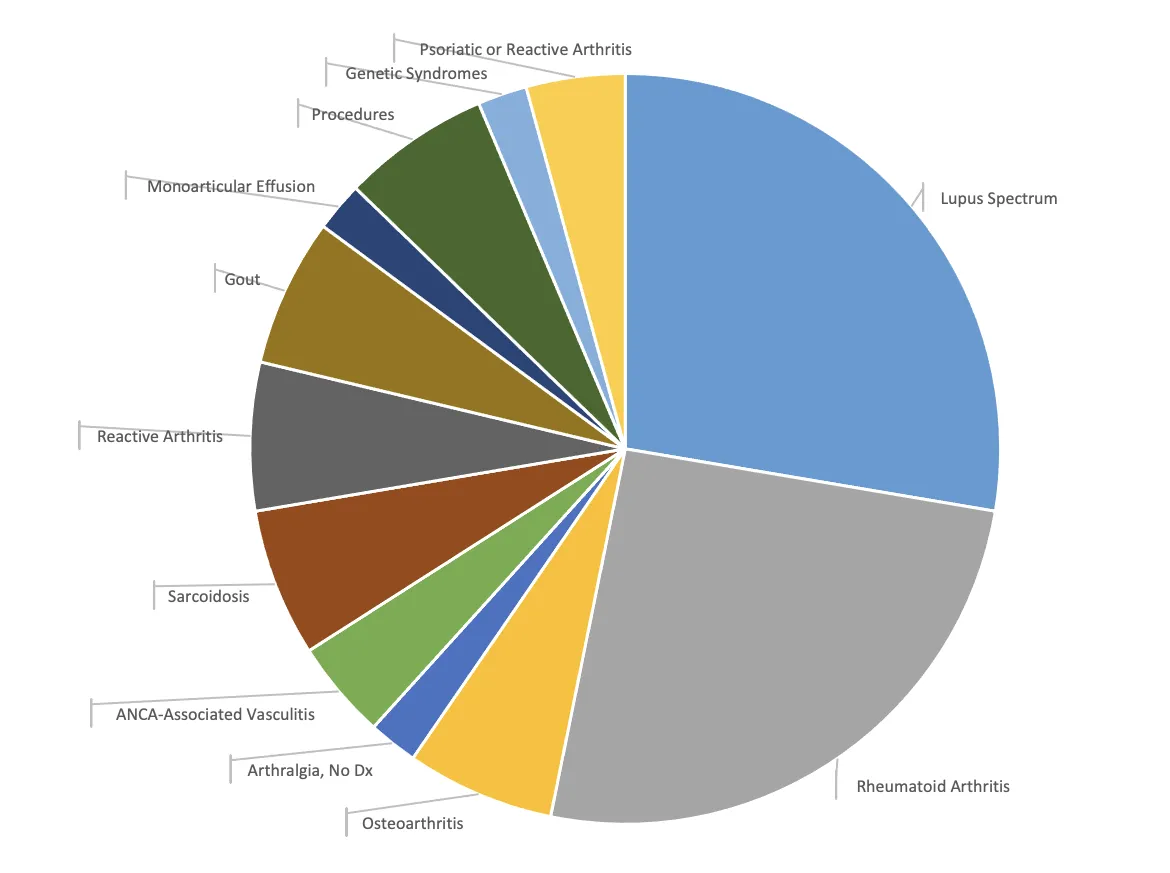
Kentucky Clinic Outpatients
Consultation Services